As the first enrollees in the Affordable Care Act begin seeking care at my hospital, I wonder how my practice as a registered nurse will change. We’re told the goal of the new law is to remodel healthcare in the United States into a system that promotes wellness and prevention, rather than just providing care to sick people. It endeavors to shift how and where healthcare is provided. Although this seems like a great objective, I worry that the switch may compromise the quality of care our patients receive.
As a bedside RN working at an acute care hospital in Oakland, California, I care for an incredibly diverse patient population: UC Berkeley professors, carpenters, stay-at-home moms, Chevron executives, and gang members. For all their various backgrounds and professions, most of my patients have had health insurance through employer-based programs, private purchase, or Medi-Cal. Most have interacted with the healthcare system prior to being admitted to my hospital.
Now, I will take care of patients who are new to healthcare. Some haven’t had care in a long time (or ever). Some may have pre-existing conditions that enabled insurance companies to refuse them coverage. Their needs may be more complicated than those of the patients I’ve been caring for throughout my career.
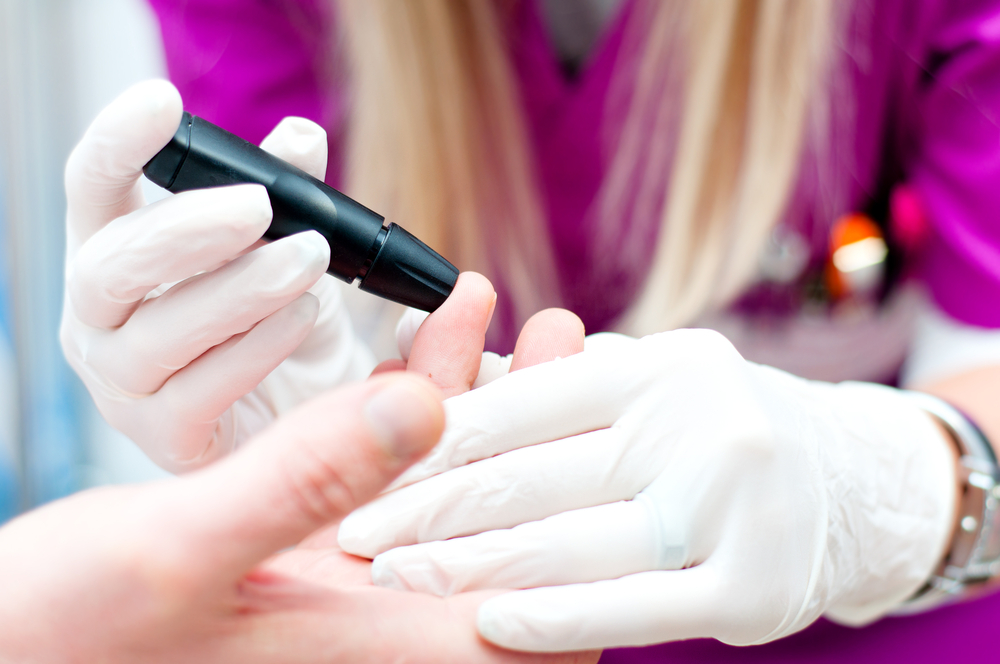
Last year, I cared for a patient who—like many patients covered through the ACA—hadn’t been to the doctor in years. After a few weeks of increasing headaches and fatigue, she came to my hospital’s emergency department and was diagnosed with Type 2 Diabetes. She didn’t have any primary care, and so we didn’t see her until she was quite debilitated by her condition. She was admitted to the hospital to stabilize her blood sugar and initiate her diabetes treatment.
Caring for this woman exemplifies the additional stress that patients who have never had healthcare may put on my hospital and nurse colleagues. This woman never had an IV in her arm, nor had she ever stayed overnight in a hospital. She closed her eyes and looked away every time I gave her an insulin injection. Now, she was told that when she went home, she’d need to check her blood sugar with a glucometer four times a day and inject herself with insulin to lower her blood sugar. She was told she needed to change her diet and exercise. The entire experience was new and bewildering for her. I spent a lot of time with her, explaining things to ease her anxiety, walking her to the bathroom so she didn’t fall.
During that shift, one of my other patients said, “You must be busy. I haven’t seen you all night.” My heart sank. He was fine physically, but I could tell he needed someone to talk to for a few minutes. Unfortunately, I had to get back to my diabetic patient. Preventing her blood sugar from dropping by ensuring she ate after each shot of insulin took priority over spending time with my lonely patient. There were no extra resources to help me with my workload, and no other nurse to care for my other patients while I spent time with this new patient.
In fact, executives at my hospital recently proposed significantly reducing our inpatient nursing staff. They say the hospital needs fewer nurses now because the number of patients admitted for overnight stays has decreased in the last few years. They say medical and surgical care has improved, and better primary care has kept patients healthy enough to avoid hospital admissions. More care is provided through home health nurses and advice nurses who answer calls from patients. There is also an expectation that the patient’s network of family and friends will assist with care. Their predictions are that the ACA will continue to bring down the number of hospital patients, which will mean even fewer nurses. The ACA permits hospitals to continue shifting patient care from the expensive inpatient setting to the cheaper—and more profitable—outpatient setting.
The problem with their diagnosis? My patients are not healthier. They continue to come to the hospital to seek care, especially when their attempts to address their symptoms through primary care fails. With the ACA, there are more patients entering hospital infrastructures that have been diminished. Patients visit the emergency room and wait longer before being admitted. When they do get admitted, rather than being sent home and told to follow up with their primary care physician, they are often much sicker and require more care.
This new burden is falling heavy on the hospitals and staff. Nurses are working harder than ever with fewer resources.
It’s a killer combination: hospitals delaying and denying care to patients as the ACA enables more Americans to buy into this deeply flawed system. If the ACA is successful in contributing to keeping patients out of the hospital, inpatient care will be reserved for patients with acute, severe illnesses, and the number of hospital nurses will drop dramatically. Meanwhile, other patients will be managed in the outpatient setting and more nurses will move into home health and advice nursing.
But it’s unrealistic to assume all the care I give my patients in the hospital can be done at home by family members, friends, and the occasional visit by a home health nurse. In a hospital, patients benefit from a huge team of healthcare practitioners who work together quickly—not only doctors and nurses, but also dietitians, physical therapists, pharmacists, wound care nurses, specialty medical doctors, social workers, and many others.
Consider my new diabetic patient. While she was in my hospital, she benefitted from the ongoing support of nurses to teach her about diabetes, visits from the dietitian to help with her menu planning, and the assistance of a social worker who helped her identify additional resources. Her doctor monitored her blood sugar to see how she responded to the treatment. The transition to her new lifestyle was going to be hard even with all our help, but it happened more quickly than if she had been sent home with that diagnosis and told to wait for the home health nurse to visit. When, after just a couple days in the hospital, she checked her sugar, determined her insulin dose, drew it up, and administered it to herself, I had tears in my eyes. It was just the kind of healthcare that I want to provide. She deserved that care, and I was proud she got it. While I hope the ACA will get care to millions of other Americans, I worry that it may make it harder for people to get the comprehensive, timely care from trained and compassionate health care practitioners, including nurses like me.



Send A Letter To the Editors